Cytomegalovirus and Herpes Simplex Virus Coinfection Neuroretinitis in an Immunocompetent Individual
The authors describe the process of distinguishing neuroretinitis from optic neuritis and vasculitis.
PF, age early 40s, was admitted to the neurology department with a 1-month history of bright scotomas that lasted for up to 1 hour with spontaneous recovery. No fever, rash, or other systemic symptoms were reported. PF had no relevant illness history, recurrent infections, medication use (including steroid use), history of substance abuse, or recent travel.
Three days after the initial event, PF had noted progressive bilateral vision loss, especially of the left eye, without headache or eye pain, and sought care from an ophthalmologist. PF, who lives in an area endemic for toxoplasmosis in northeast Brazil, had positive toxoplasmosis serology, and empiric antibiotic treatment for toxoplasmosis was initiated. Doxycycline also was started in anticipation that other infectious agents may have been present. However, no clinical improvement occurred, and a new finding of bilateral optic disc edema (Figure 1) led PF to seek emergency care at the authors’ hospital, a tertiary general hospital focused on neurologic cases and stroke in northeast Brazil.

Diagnostic Process and Studies
On presentation to hospital, severe vision loss (visual acuity 20/800 in the left eye and 20/70 in the right eye) with a pupillary afferent defect in the left eye was noted. The initial fundoscopic examination revealed worsening of bilateral optic disc edema (Figure 2), and 5 days later, fundoscopy showed signs of retinal vasculitis and arteriovenous shunts (Figure 3).


The clinical scenario worsened over the following days. A head CT was performed, yielding normal results. Cerebrospinal fluid (CSF) analysis showed mild inflammation with 7 cells/mm³ and protein level 49 mg/dL. Head MRI could not be performed initially because of patient-reported claustrophobia. Fluorescein angiography and optical coherence tomography revealed retinal vasculitis (Figures 4, 5). In this context, a diagnostic hypothesis of inflammatory optic neuritis was proposed. A wide investigation was performed; no clinical signs of systemic vasculitis or fever were present, and rheumatologic disease markers were negative, ruling out autoimmune (antineutrophil-cytoplasmic antibody [ANCA]) diseases, systemic lupus erythematosus, and Sjögren syndrome. PF had no signs of tuberculosis, which is endemic in Brazil. Therapy was initiated with intravenous methylprednisolone 1 g/d for 4 days on the basis of the hypothesis of autoimmune optic neuritis associated with retinitis and retinal vasculitis. No improvement occurred.


During the investigation, multiple lumbar punctures were performed, and an elevated CSF opening pressure (30 cm H2O) was sustained. Because of the lack of clinical response to immunosuppression, acetazolamide 750 mg/d was prescribed, which later was switched to topiramate 100 mg/d because of elevated transaminase levels.
Severe vision loss remained despite the initial therapy. Two weeks after presentation, a head MRI study was performed with sedation. No indirect signs of intracranial hypertension were present. The MRI scan showed extensive left optic neuritis, and the vessel wall sequence detected signs of central nervous system (CNS) vasculitis involving both middle cerebral arteries and the left posterior cerebral artery (Figure 6).
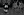
PF was evaluated by an ophthalmologist, who documented development of a macular star on retinography, resulting in a definitive diagnosis of neuroretinitis. Further serologic tests, performed 40 days after initial symptoms, were positive for herpes simplex virus (HSV) and cytomegalovirus (CMV). HSV serology showed positive immunoglobulin M and negative immunoglobulin G; CMV was positive for both immunoglobulin G and immunoglobulin M. Enzyme-linked immunosorbent assay did not detect human immunodeficiency virus (HIV) antibodies.
Case Resolution
Initial treatment consisted of intravenous acyclovir 10 mg/kg every 8 hours; 14 days after CMV serology results were received, the treatment was switched to intravenous ganciclovir 5 mg/kg every 12 hours. HSV and CMV polymerase chain reaction were not available in the authors’ hospital because of cost constraints. A slow and progressive clinical response was achieved after 4 days (Figure 4), and PF was discharged home with oral steroids with progressive tapering.
Over a 3-month follow-up, PF had marked improvement in retinography results in both eyes. Visual acuity was improved in the right eye. The left eye had only subjective improvement, showing signs of possible sequelae (visual acuity 20/30 in the right eye and 20/400 in the left eye).
Discussion
PF exhibited findings visualized on MRI scans indicative of optic neuritis; however, the presentation was atypical for inflammatory optic neuritis, and there was no improvement seen with administration of steroid therapy. These factors prompted further investigation into infectious etiologies of optic neuritis and neuroretinitis. Subsequent examinations revealed positive serology for both CMV and HSV.
Neuroretinitis was considered as a diagnosis because of optic neuritis secondary to CMV and HSV coinfection, with associated features of retinal and CNS vasculitis. The inflammatory course in the CNS contributed to elevated intracranial pressure, with no other identifiable causes for the increased intracranial pressure.
Neuroretinitis—a neurologic disorder characterized by optic disc edema, unilateral vision loss, and a macular star pattern—is commonly attributed to infectious causes. Bartonella species and viruses, particularly CMV and HSV, are frequent culprits. Our case is noteworthy for its uncommon bilateral manifestation and positive serologies (CMV and HSV) in an immunocompetent adult.1
CMV can manifest in various ocular forms, such as retinitis, neuroretinitis, papillitis, or optic neuritis. CMV retinitis was first described in 1964, with increasing numbers of cases being diagnosed with the advent of immunosuppressants and more markedly in the context of the AIDS epidemic.9 CMV retinitis is the most common cause of visual loss in people with HIV infection, but this correlation is not present in immunocompetent individuals. Although typically associated with immunosuppression and exhibiting a progressive and severe course, CMV retinitis generally responds well to antiviral treatment.2 In some immunocompetent individuals, as observed in our case, atypical clinical features may include marked arterial vasculitis and chronic retinal necrosis.3 Cases not associated with HIV infection have been noted to involve marked vitritis and vascular occlusion beyond the site of retinitis.4
HSV can present with diverse visual symptoms, especially in the context of acute retinal necrosis, which may involve occlusive vasculopathy. Our case was distinct from acute retinal necrosis because of the absence of retinal necrosis.
Diagnosis of herpetic ocular and CNS infections is usually made by polymerase chain reaction, which can be performed using CSF or intraocular sampling. Serologic testing has limited specificity, considering the lack of pathologic correlation. Nevertheless, the intraocular pattern along with clinical and radiologic improvement supported the clinical reasoning.5
A case similar to ours was reported in Thailand, in which an individual, age late 40s, was diagnosed with neuroretinitis attributable to CMV and HSV coinfection after experiencing visual changes in the left eye for 3 days. This individual was treated with 2 weeks of intravenous ganciclovir and experienced considerable improvement.7 PF had a less successful visual outcome because of late diagnosis and lack of the technology needed to provide a more accurate and timely diagnosis.
There are reports in the literature of cases of retinal HSV and CMV coinfection in immunosuppressed individuals.6 Our case is unique in that it presents HSV and CMV coinfection in an immunocompetent individual with neuroretinitis and CNS vasculitis, resulting in a rarer and potentially more serious scenario. CMV and HSV coinfection in an immunocompetent individual has been reported previously in the setting of systemic disease and was treated successfully with valacyclovir.8
Ready to Claim Your Credits?
You have attempts to pass this post-test. Take your time and review carefully before submitting.
Good luck!
Recommended
- Imaging & Testing
MRI Clues to Intracranial Infection: Differentiating Bacterial, Viral, Fungal, and Parasitic CNS Disease
Márk Kozák, MD; Máté Sik, MDMárk Kozák, MD; Máté Sik, MD - Imaging & Testing
Artificial Intelligence in Clinical Neurology: Opportunities, Limitations, and the Path Forward
Aysha Jadran, MD; Saqib A. Chaudhry, MDAysha Jadran, MD; Saqib A. Chaudhry, MD



