Case Conference: The “Noise” of Medicine
In this article, we use the term “noise” not to refer to the literal noise of a busy emergency department on a Saturday night, but rather, to refer to the statistical concept of “noise.” Specifically, we focus on “occasion noise,”1 which arises whenever the accurate responses to the same question vary with factors that are, from a logical point of view, irrelevant to the question asked.
In an ideal world, the accuracy of medical diagnosis would not depend neither on how busy the emergency department is at the time of diagnosis, what the doctor had for breakfast, whether it was humid or not that day, what the previous patient’s diagnosis was, nor myriad other considerations not germane to the clinical scenario. Human performance, however, does perforce depend on many such irrelevant factors, although we are only vaguely aware of their impact. Sleep deprivation, for example, slows reaction time and induces “unstable and unpredictable patterns of behavior.”2 Thus, it is unsurprising that a high level of sleep deprivation is associated with nearly doubled rates of self-reported medical errors.3
More surprising examples of occasion noise, collected by psychologist Daniel Kahneman and colleagues in, Noise: A Flaw in Human Judgment,1 include doctors’ prescription patterns varying with time of day; judges’ decisions of rejecting political asylum being more likely when the 2 prior asylum requests were approved; college admission officers’ ratings of applicants varying with cloud cover on the day of decision, and more.1
Checklists to the Rescue!
It is easy to appreciate that occasion noise is unwelcome in medicine. Inconsistent delivery of the high level of care that clinicians are capable of increases rates of undesirable outcomes (eg, opioid addictions, missed diagnoses, or procedural complications). Are there any practical tools for reducing occasion noise in the fast-paced medical setting? An easy-to-use, low-tech tool that has received increasing attention is an old-fashioned checklist: “a list of items required, things to be done, or points to be considered, used as a reminder.”4
Checklists, of course, are not new to medicine. A traditional differential diagnosis is a kind of checklist designed to educate and to reduce diagnostic occasion noise; the differential reminds clinicians not to miss aortic dissection or pulmonary embolism in a patient with shortness of breath and chest pain.
The chief difficulty in applying a differential diagnosis checklist is that it presupposes that practitioners know which checklist to apply, (ie, they are able to formulate the clinical problem correctly). This may be relatively straightforward in a patient with crushing chest pain but oftentimes it is not.
Consider a patient presenting with weakness in the arms but not the legs. The hardest part of the cognitive process may be recognizing this presentation as consistent with “man-in-a-barrel syndrome.” Once this syndrome is recognized, the clinician is well on the way to arriving at the correct diagnosis because the differential for the man-in-a-barrel syndrome is relatively short: bilateral watershed infarctions between the anterior and middle cerebral artery (MCA) territories, central spinal cord compression, anterior horn cell disease (eg, amyotrophic lateral sclerosis [ALS]), and a few more exotic conditions.5 Clinical context and imaging findings usually allow the clinician to pick the diagnosis from this list that best fits the case.
Moreover, even the right checklist does not always contain the right answer. Even the most comprehensive differential diagnosis checklist is never exhaustive. In a recent case report, the man-in-a-barrel syndrome was attributed to cord tethering in the setting of postinfectious adhesive arachnoiditis.6 This unexpected possibility has not been explicitly considered in the review articles on the topic.5 Another example of “checklist failure” from our practice involved a previously healthy person who developed brain lesions, retinopathy, and deafness in midlife. We surmised that he had a disorder on the differential of brain-eye-ear diseases (BEE syndrome),7 yet extensive workup was inconclusive. After years of diagnostic uncertainty, he underwent whole-exome genome screening, which revealed genetic mutations consistent with hemoglobin SC disease. Although Hb SC disease has not been traditionally regarded as a “BEE disease,” it explained the unusual constellation of symptoms.8
The following case from our practice illustrate a different kind of problem that may be encountered when deploying a differential diagnosis checklist in real life.
Video. AW had flexed posture of the left arm (A) and low-amplitude, high-frequency asymmetric tremor, predominantly of the right extremities (B). Differences in gait on the left vs right side were seen.
Diagnosis
The chief difficulty of applying the checklist approach in this case is that the findings do not “add up.” There is evidence of parkinsonism, predominantly on the right side, and spastic hemiparesis on the left. Which checklist should we use? We could look for obscure disorders that can cause both parkinsonism and spastic hemiparesis—perhaps a hemiparetic form of Parkinson disease?9 The more likely scenario is that AW has 2 relatively common neurologic conditions: Parkinson disease and a brain lesion along the right corticospinal tract. AW’s brain MRI (Figure 2) showed findings consistent with chronic right frontotemporal infarction with insular involvement and scattered foci of subcortical hyperintensities suggestive of small vessel ischemic cerebrovascular disease. AW’s final diagnosis was Parkinson disease in a person with a right MCA stroke.
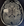
Figure 2. AW’s brain MRI showed a right frontotemporal lesion, consistent with infarction with insular involvement and scattered foci of subcortical hyperintensities, consistent with small vessel disease.
Pause Points Make Strong Checklists
In The Checklist Manifesto,10 Dr. Atul Guwande outlines conditions for a successful checklist. The checklist should be reasonably concise (preferably <10 items); use simple and precise language; and have a clearly defined “pause point” at which it is to be deployed. Regarding differential diagnosis checklists, the pause point comes after the relevant data has been collected and an adequate clinical formulation proposed. In contrast, diagnostic criteria for a specific disorder, or the “3-for-5” heuristic discussed in our previous columns,11-13 are different kinds of diagnostic checklists that should be deployed at a later pause point: when you already have a good idea of the likely diagnosis and need to check how well it fits the case. For maximal effectiveness, checklists should be custom-built for the individual’s practice. For example, The Multiple Sclerosis Lesion Checklist14was designed to be deployed when assessing the likelihood of demyelinating disease at the time of brain MRI evaluation in a patient with transient neurologic symptoms.
Conclusions
Considering the high prevalence of “occasion noise” in medicine and the proven utility of checklists across different fields, medical practitioners should be encouraged to adopt and adapt checklists for commonly encountered clinical scenarios and try them out in their everyday practice. Importantly, checklists are not meant to replace a holistic, intuitive approach to case assessment, but only to supplement it. Like all tools, checklists have limitations. Experience and clinical acumen are needed to determine which checklist to apply in each individual case. The possibility of dual diagnoses needs to be borne in mind when clinical symptoms do not “add up;” and differential diagnoses should always include a “none of the above” option. Despite these caveats, well-formulated diagnostic checklists with clear pause points can be invaluable in helping clinicians maintain a consistently high level of diagnostic performance.
Ready to Claim Your Credits?
You have attempts to pass this post-test. Take your time and review carefully before submitting.
Good luck!
Recommended
- Imaging & Testing
MRI Clues to Intracranial Infection: Differentiating Bacterial, Viral, Fungal, and Parasitic CNS Disease
Márk Kozák, MD; Máté Sik, MDMárk Kozák, MD; Máté Sik, MD - Imaging & Testing
Neuroimaging: Clinical Impact of Imaging Findings
Laszlo Mechtler, MD, FAAN, FEAN, FASN, FAHSLaszlo Mechtler, MD, FAAN, FEAN, FASN, FAHS - Imaging & Testing
Neuroimaging After Brain Radiotherapy and Radiosurgery
Venkatesh Shankar Madhugiri, MBBS, MCh, FACS; Neil D. Almeida, MDVenkatesh Shankar Madhugiri, MBBS, MCh, FACS; Neil D. Almeida, MD



