Incorporating Cultural Considerations Into Neuropalliative Care
Neuropalliative teams can meet the cultural needs of individuals and families through transdisciplinary collaboration.
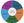
People navigating serious neurologic illness and their care partners experience multidomain suffering.1 For neuropalliative providers, this suffering is explored and understood through a care model focusing on the discrete domains informing the experience (Figure 1). Assumed cultural norms that inform provider expectations for care and suffering do not generalize across cultures. In the United States, the patient or an identified surrogate is expected to coordinate care and make independent decisions. In addition, persisting health care disparities that disproportionately affect individuals from underrepresented racial or ethnic groups directly contribute to and exacerbate the suffering that neuropalliative care aims to improve.2
To achieve person-centered care, neuropalliative providers must apply a culturally considerate lens to their care: first, through recognition of the various stressors that affect the patient and their family; second, through humble inquiry of the patient’s and care partners’ approaches to navigating these stressors.3 Failure to recognize, respect, and respond to the cultural practice of individuals and families navigating serious illness risks mistrust, perception of discriminatory behavior, and decreased adherence to care recommendations.4 Culturally considerate neuropalliative care emphasizes collaboration between the individual and the provider to identify care preferences. As neuropalliative care is increasingly highlighted by specialty organizations and advocacy groups,5 neuropalliative providers are uniquely positioned to model the provision of culturally considerate neuropalliative care.
A distinguishing feature of neuropalliative care is the appreciation for the unique set of symptoms experienced by people with severe neurologic illness.1 Recognition for how individuals and their care partners arrive at decisions, particularly in the context of the existing inequities that inform their medical experiences, offers unique opportunity for members of a neuropalliative care team to address these multidomain needs in the manner necessary and appropriate for the neurologic condition. In this article, we offer an approach to empower neuropalliative teams to meet the cultural needs of patients and families through transdisciplinary collaboration (Figure 2).

Disease-Specific Cultural Considerations in Delivering Neuropalliative Care
Stroke and Severe Acute Brain Injury
Known Palliative Care Needs and Existing Disparities. Stroke is a leading cause of death and disability.6 Clinicians providing care for people who have had a stroke require skill delivering serious news, responding to emotion, prognostication, and care planning, particularly in the acute setting.7 Neuropsychiatric symptoms are heterogeneous and often underrecognized, and thus require careful monitoring in the postacute period.8 Surrogate decision-making is common in the acute setting, and care planning is critical after injury. There are well-described disparities observed at each point along the continuum of stroke care, from prehospital symptom recognition to acute treatment to postinjury care.7 Numerous disparities exist, including differences among White, Black, or Hispanic individuals in transfer to endovascular-capable centers, and functional outcomes as measured by modified Rankin Scale scores.7
Opportunities for Transdisciplinary Neuropalliative Care. Decision-making frequently falls on surrogate decision-makers at unexpected times. They process information and arrive at decisions in the context of their personal and cultural experiences navigating health care. Differences in palliative care use across racial or ethnic minority groups in hospitals are attributed both to provider- and organizational systems-level recognition of palliative care needs.9,10 Recognition of how care partners arrive at decisions may inform opportunities for a team to align with families upstream of when decisions need to be made, offering decision-makers the opportunity to process new information with a supportive community.
A transdisciplinary approach can facilitate the recognition and addressing of neuropalliative care needs.11 This equips any member of the neuropalliative team to take a cultural history, followed by a team evaluation to identify the clinicians best equipped to lead the intervention (Table 1). For example, a nurse, advanced practice provider, or physician taking a cultural history may learn that prayer is key for a family to make decisions, and that the care partners have lost access to prayer in the acute setting. The neuropalliative team may determine that the chaplain is best equipped to lead the team in addressing the spiritual or existential distress experienced by the family. In this example, the nurse or physician screening for spiritual distress invites the family to express their cultural preference in a medical scenario in a manner in which they may not have otherwise felt empowered. This invitation builds rapport and facilitates high-quality communication of needs between the medical team and family.12

Parkinson Disease and Related Disorders
Known Palliative Care Needs and Existing Disparities. There is high burden of symptoms in Parkinson disease (PD) and related disorders (PDRDs), including motor and nonmotor symptoms.13 Nonmotor symptoms span physical, cognitive, emotional, and spiritual domains. The chronic and progressive nature of PDRD results in variable and cumulative palliative care needs in both patients and care partners. Families and providers alike describe limitations addressing these needs.13,14 PD is underrecognized in people from underrepresented racial or ethnic groups.15 Whereas age is regarded as a primary risk factor for PD, structural and environmental risk factors disproportionately affecting people from underrepresented racial or ethnic groups have been found.16 Underrecognition of prodromal symptoms delays diagnosis and may account for differences observed in motor, nonmotor, and quality of life scales in Black compared with White individuals,17 having staggering effects on patients and care partners for these progressive illnesses measured in years to decades.
Opportunities for Transdisciplinary Neuropalliative Care. Culturally competent care in PD centers on considerate communication strategies and recognition of a patient’s support network. Provider recognition and inquiry regarding how a family prefers communication and care planning may facilitate honest discussion and increase the likelihood of follow-up discussions,18 which are necessary as the priorities are likely to shift as the illness progresses. Strategies may focus on dedicated medical visits to inquire about existing supports for the patient and family, or use of separate encounters with a nurse or social worker to inquire about how the care network makes decisions.19 This latter approach to “road-mapping” discussions may prove valuable in communities where decisions are made in a group, as opposed to an individual. In the outpatient setting, interdisciplinary team members who initiate or guide conversations around care planning offer opportunities for family to discuss priorities they may have considered outside the scope of a physician-led medical visit.
Dementia
Known Palliative Care Needs and Existing Disparities. Dementia encompasses numerous pathophysiologic origins (eg, Alzheimer disease, cerebrovascular disease, and alpha-synucleinopathies, including parkinsonism). They vary in their upstream clinical presentations before a common pathway of progressive functional loss, cognitive dysfunction, and physical debility. Identified palliative needs include unique symptom burden (eg, neuropsychiatric symptoms, dysphagia and aspiration, debility), upstream caregiver role strain, and challenges around advance care planning due to prognostic uncertainty.19,20 A study evaluating timeliness to dementia diagnosis revealed differences in time to diagnosis and comprehensiveness of diagnostic evaluation across racial groups, even after controlling for physical and regional confounds.21 A separate viewpoint highlighted the consequences of using race as a proxy for social determinants of health in neuropsychologic testing; this resulted in differences around diagnosis, interpretation of illness severity, and access to available resources.22
Opportunities for Transdisciplinary Neuropalliative Care. There are limited studies on the prevalence of specific neuropsychiatric symptoms in people with dementia from underrepresented racial or ethnic groups. Neuropsychiatric symptoms, including depression, hallucinations, disinhibition, and apathy, are common in people with dementia across racial or ethnic groups, although some studies report differences in how people from different groups report or manage these symptoms.23,24 Strategies among caregivers to cope with these challenging symptoms vary with cultural context. This represents opportunities for upstream anticipatory guidance by interdisciplinary team members, beginning with gentle inquiry into how families approach symptoms in these conditions, offering opportunities for families to share their preferences outside of a physician-led visit. Physicians equipped to screen the aforementioned domains are encouraged to do so early after diagnosis, in order to establish an open environment for consideration of cultural preferences in the care patients will continue to receive.
End of Life in Severe Neurologic Illness
Known Palliative Care Needs and Existing Disparities. Compared with people with cancer, people with neurodegenerative disease are more likely to visit the emergency department and less likely to use hospice services at the end of life.25 A study exploring end of life in PD found the intensity of hospitalization to vary by race, ethnicity, and geographic location.26 These experiences represent opportunities for palliative care use. However, limitations in access to palliative care remain. In Alzheimer disease and related dementia with high mortality risk, inpatient hospitalization best correlated with affluence, access to a teaching hospital, and non-Hispanic White race.27 In older individuals presenting with severe traumatic brain injury, presence of a do-not-resuscitate order at hospital admission differed between racial groups; presence of a do-not-resuscitate order was also associated with increased rate of discharge to hospice and reduced hospital length of stay.28 The disparities persist in hospice, with differences in the rate of disenrollment from hospice across racial and ethnic groups for individuals with dementia.28
Opportunities for Transdisciplinary Neuropalliative Care. High-quality communication, inquiry into perceived experiences of suffering, and appreciation for heterogeneity in the process of decision-making have great effect.3 Culturally specific educational programming reduces differences in attitudes concerning advance care planning.18,29,30 An approach that involves collaboration between team members and key community members facilitates quality collaboration that more directly identifies and meets expressed community needs.29,31,32
Discussion
In this article, we highlight how a team-based approach can facilitate culturally considerate neuropalliative care. We describe opportunities for a transdisciplinary neuropalliative care team to incorporate cultural history-taking into their needs assessments, with a flattened hierarchy enabling the best-equipped team member to lead the collaboration with the patient and family.
There are multiple strengths to this approach. First, we recognize that individuals and families present to medical contexts with varied personal experiences, informing their beliefs on what is discussed in medical visits. Second, we highlight the importance of a transdisciplinary approach to group visits. Transdisciplinary medical visits reduce the perception of hierarchy within the medical team, and empower the team to focus visits on the most pertinent needs of the patient and family.33 An environment in which any team member can direct discussions unique to the needs of chosen family members can facilitate candid conversation that may otherwise take more time in a physician-directed visit. Similarly, having physicians and nurses take a cultural history and screen for distress in the psychological, social, and spiritual domains signals to patients and families that these areas hold significance to the medical team, further aligning with the patient’s and family’s needs.34 This approach is adaptable to conditions commonly seen in the inpatient (eg, severe acute brain injury) and outpatient (eg, PDRD, Alzheimer disease and related dementia, amyotrophic lateral sclerosis, multiple sclerosis) settings.33,35,36
We also recognize challenges with this approach. First, settings with the resources to deliver transdisciplinary neuropalliative care are likely limited to high-resource settings, such as academic referral centers, limiting the generalizability of this approach to community settings. In these instances, we further highlight the value of this interdisciplinary approach (Figure 1), where providers with diverse clinical training backgrounds are equipped with the knowledge and skills to identify care needs across domains and initiate conversations about available resources to meet those needs. Second, interprofessional collaboration requires explicit conversation among disciplines, particularly around the extent to which they can initiate conversations outside of their traditional practice.37 We view these conversations between clinicians as opportunities to empower one another to meet the needs of patients and families in the moment, and to facilitate opportunities for clinicians to learn from one another.
Neuropalliative care inherently centers the experience of patients and their care partners, identifying and addressing multidomain distress and facilitating discussion through high-quality communication. There is urgency to identify interventions to address disproportionate mortality rates across cultural groups.38 By empowering team members, including physicians, to participate in an interdisciplinary and transdisciplinary care model, teams can improve quality communication, and invite culturally diverse patients and families to engage in whole person–centered medical care.
Ready to Claim Your Credits?
You have attempts to pass this post-test. Take your time and review carefully before submitting.
Good luck!
Recommended
- Imaging & Testing
Neuroimaging: Clinical Impact of Imaging Findings
Laszlo Mechtler, MD, FAAN, FEAN, FASN, FAHSLaszlo Mechtler, MD, FAAN, FEAN, FASN, FAHS - Alzheimer Disease & Dementias
Special Report: 2025 Neurology FDA Drug & Device Approvals & Clearances
- Imaging & Testing
Neuroimaging Biomarkers in Alzheimer Disease and Related Dementias: From Structural MRI to Amyloid and Tau PET
John Bertelson, MD; Bela Ajtai, MD, PhDJohn Bertelson, MD; Bela Ajtai, MD, PhD



