Procedural Treatments for Headache Disorders
In persons with headache disorders for whom oral therapeutics are inadequate, poorly tolerated, or contraindicated, procedural options should be considered. Procedures can be abortive and/or preventative, as well as diagnostic in some cases. These treatments also vary in invasiveness ranging from peripheral nerve blocks to surgical decompressions. Procedures can be used independently or with oral pharmacologic and nonpharmacologic treatment options.
Botulinum Toxin
OnabotulinumtoxinA (BTX) was the first treatment approved by the Food and Drug Administration (FDA) for the prevention of chronic migraine (CM). In clinical trials, participants were injected every 12 weeks for 24 weeks with 155 units into fixed injection sites with an optional additional 40 units injected if pain continued.1
Although up to 49% of individuals treated can have a 50% reduction in headache days after the first round of injections, 11% and 10% of patients respond only after their second and third rounds of injections, respectively.2 The beneficial effect of BTX on CM is thought to occur through BTX blocking the release of neuropeptides implicated in migraine. Furthermore, BTX can reduce peripheral sensitization and reverse central sensitization over time, which has been implicated in CM progression.3
Given the limited contraindications and drug interaction profile of BTX, it is an ideal choice for individuals with migraines that do not respond to oral medications or those who have contraindications to or difficulty tolerating oral medications. Side effects following BTX injections include temporary neck pain, headache, muscle weakness, and ptosis. Contraindications include pregnancy and certain neuromuscular disorders, such as myasthenia gravis.2,4
The current standard FDA-approved paradigm involves 31 injections into specific muscle groups (ie, corrugator, procerus, frontalis, temporalis, occipitalis, cervical paraspinal, and trapezius) (Figure 1).3,5
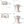
It is important to assess patients for other conditions that potentially can exacerbate migraine, such as temporomandibular disorders (TMD) and cervical dystonia. The prevalence of TMD is higher in individuals with CM compared with the general population.6 An effective treatment option for patients with CM and concomitant TMD can include injection of BTX to each masseter muscle.7
Clinicians should be aware of a few pitfalls that can occur with BTX treatment. Ptosis is more likely with injections in the frontalis that are too close to the eyebrows and too far laterally from the mid-pupillary line. Neck pain is more likely to occur with injections that are performed too inferiorly in the neck. Injecting superiorly in the frontalis and neck will help to avoid these issues. Ptosis can also occur if corrugator injections are performed in the wrong location, and a double dose is delivered to the adjacent frontalis. This can be avoided by pinching the corrugators between the fingers of the noninjecting hand and performing injections parallel to the muscle fibers.

Whenever initiating a new preventative treatment, maintaining headache diaries is essential in order to gauge improvement of headache with some degree of precision. Patients will frequently claim no response subjectively, but a careful review of diaries can demonstrate an improvement of both headache frequency and intensity that tends to progress with subsequent BTX treatments. Injections should be performed every 12 weeks, because delays in treatment can lead to worsening of headaches between injection cycles. In a busy practice, it is not uncommon for patients to have standing 12-, 24-, and even 36-week appointments scheduled in advance to ensure timely BTX treatments. Some individuals will start having reminder headaches during weeks 10 to 11—experiencing a transient spike in headaches—then realize that they have an appointment for BTX treatment the next week. In addition to personal circumstances and clinic issues, pharmacy and delivery issues can cause delays in BTX treatment, so it is important that the patient and staff communicate effectively regarding ordering and delivery of BTX when dealing with specialty pharmacies.
Peripheral Nerve Blocks
Peripheral nerve blocks (PNBs) involve injecting local anes-thetic, with or without steroid, in the distribution of a specific nerve and can be safely performed in the office to treat numerous headache disorders. Commonly used blocks in headache medicine include occipital, supraorbital, supratrochlear, auriculotemporal, and sphenopalatine ganglion blocks. Overall, PNBs are well tolerated with limited side effects that can include injection site pain, numbness, and lightheadedness.8 In individuals for whom polypharmacy and potential drug interactions are an issue or for whom certain headache medications are contraindicated, PNB can be a safe and effective therapeutic option.9 The use of steroids can lead to skin atrophy and hair loss at the injection site, typically only when serial injections are given in the same location. For this reason, injections with steroid should be avoided in cosmetically sensitive areas such as the face, where atrophy can be disfiguring.10
Migraine and Cluster Headache
Studies have shown that PNB, particularly occipital nerve blocks, can be effective for preventive and acute treatment of migraine or status migrainosus, which can be particularly useful for treating headaches in emergency department and urgent care settings.11 Other indications that can prompt trigeminal nerve blocks include supraorbital tenderness and prior injection response. A study of 70 women with migraine reported that 80% had reduction in acute symptoms with supratrochlear and supraorbital blockade.8,12 Injection of the ipsilateral occipital nerve with steroid has shown to be effective at terminating a cluster headache cycle.13
Occipital Neuralgia
Occipital nerve blocks (ONB) can be both diagnostic and therapeutic.14 Occipital neuralgia is a recurring, severe, unilateral or bilateral, paroxysmal shooting or stabbing type pain in the distribution of the occipital nerves. The pain can be associated with altered sensation and/or cutaneous allodynia.

Although there is limited data regarding the prevalence of occipital neuralgia, a community-based headache clinic study estimated that up to 25% of patients presenting with a chief complaint of headache had occipital neuralgia. Among persons with occipital neuralgia, 85% had a coexisting headache disorder, most commonly CM, suggesting that occipital neuralgia may exacerbate the concurrent headache disorder. Identification and adequate treatment of occipital neuralgia with ONB is the standard of care in such cases.15
Other Focal Neuralgias
In addition to occipital neuralgia, some patients will also present with supraorbital neuralgia, supratrochlear neuralgia, and/or auriculotemporal neuralgia. Trauma is a common cause of these focal cranial neuralgias, but they can also occur spontaneously. In clinical practice, larger volume nerve blocks tend to be more effective for the treatment of focal neuralgias. A possible mechanism of action is that larger volume injections are actually causing an expansion of some of the different tissue planes, which can lead to the decompression of entrapped peripheral nerves.
Similar nerve decompression may occur in persons who undergo the set of procedures referred to as migraine trigger site deactivation surgery. For those who respond positively to surgery, it is possible they had a focal neuralgia in addition to migraine, and decompression of the neuralgia led to resolution of the neuralgia, and subsequent improvement of migraine.16
Technique
According to the American Headache Society Interventional Procedure Survey (AHS-IPS), there is much variation in physicians’ views regarding the indications for PNB, as well as medications used, volumes injected, and techniques. The most commonly used anesthetics are lidocaine and bupivacaine.8 The Procedural Headache Medicine Section of the American Headache Society published expert consensus recommendations in an attempt to provide guidelines for performing PNB.10
Occipital Nerve Block. The greater occipital nerve is localized as the point at the proximal third of a line from the inion to the mastoid process (Figure 2).

Supraorbital and Supratrochlear Nerve Blocks. To localize the supraorbital or supratrochlear nerve, the supraorbital ridge is identified by palpation and the site of needle insertion is superior to the ridge (Figure 3).

Auriculotemporal Nerve Block. The auriculotemporal nerve is localized by palpating the temporal artery at the level of the tragus and moving 2 fingerbreadths anterior and superior (Figure 4).

Sphenopalatine Ganglion Block. Sphenopalatine ganglion (SPG) blockade can be achieved with various approaches. The least invasive is the intranasal administration of anesthetic to the nasal mucosa vs a more invasive injection through the cheek with fluoroscopic guidance. Traditionally the procedure was performed with a cotton-tipped applicator immersed in a concentrated local anesthetic, such as lidocaine, 4%, and applied to the posterolateral wall of the nasal cavity. The patient is positioned supine and the head turned toward the side of application during insertion of the anesthetic.17 Simpler methods now exist with the use of devices that allow for a small, flexible catheter to be advanced into the nasal cavity and delivery of local anesthetic, such as bupivacaine, 0.5%, to the posterolateral wall of the nasal cavity. This technique not only allows the patient to remain upright for the procedure but also takes less time to administer and results in less discomfort.
Trigger Point Injections
Frequently, persons with chronic headache disorders complain of muscle pain and tightness. Occasionally on physical examination the pain may be reproducible, and individuals are diagnosed with myofascial pain or muscle spasm. Trigger point injections (TPI) with anesthetic are frequently utilized to relieve such myofascial pain. Identifying the trigger points is done by palpating the muscles of the head and neck and identifying reproducible areas of pain and/or identifying tight muscle bundles or knots as some patients would call them. The trapezius muscle and the sternocleidomastoid are the most common and second most common trigger points encountered in persons with headache disorders, respectively.
The injection site will be the area where the tight muscle band has been identified, or the area of most reproducible pain. After the affected muscles are identified, the area should be cleaned with alcohol. The injection site should then be stabilized with the noninjecting index finger and thumb, and the needle inserted into the skin and advanced at a 30-degree angle into the trigger point. Prior to delivering anesthetic, pull back the plunger to ensure no blood return. Similar to PNB, there is variation among clinicians in regard to the gauge of the needle, volume injected, and anesthetic used. The most commonly used anesthetics are lidocaine or bupivacaine. There is limited efficacy data regarding trigger point injections; however, it is a treatment that is frequently used in addition to PNB to manage the headaches and associated neck pain/spasm.8,18
Conclusion
The use of procedures in headache medicine can effectively augment or at times replace conventional pharmacotherapy. In patients with contraindications, poor tolerance, or inadequate efficacy with oral medications, these procedures are useful options. Whereas some interventions are more invasive, most procedures can be safely performed in the office, require little to no downtime, and are viable tools in the headache armamentarium.
Ready to Claim Your Credits?
You have attempts to pass this post-test. Take your time and review carefully before submitting.
Good luck!
Recommended
- Imaging & Testing
MRI Clues to Intracranial Infection: Differentiating Bacterial, Viral, Fungal, and Parasitic CNS Disease
Márk Kozák, MD; Máté Sik, MDMárk Kozák, MD; Máté Sik, MD - Imaging & Testing
Neuroimaging: Clinical Impact of Imaging Findings
Laszlo Mechtler, MD, FAAN, FEAN, FASN, FAHSLaszlo Mechtler, MD, FAAN, FEAN, FASN, FAHS - Imaging & Testing
Practical MRI in Neurology: Use Cases, Technologies, and Opportunities for Outpatient Clinics
Joseph Fritz, PhD; Edmond A. Knopp, MD, DABR, FASFNRJoseph Fritz, PhD; Edmond A. Knopp, MD, DABR, FASFNR



